
Warning: This is a LONG post. If you or someone you know has suffered this rare injury, I hope it helps. That’s pretty much the point of it. The post will bore everyone else. This is the first of 3 parts. Part 2 covers weeks 2-6. In part 3, I talk about Mark’s experience during weeks 6-12.
It’s important to note that your experience might be completely different depending on your ability to rehab at home after the surgery, your age, weight, whether you have someone at home with you 24/7 (our situation) and the type of repair that was done. Mark did not require cadaver tendons which might have affected the healing timeline on the front end.
This post contains affiliate links to products we used (and are using). If you purchase a product I receive a small commission at no additional cost to you. I took the time to include links for your convenience, too. You probably have a lot going on.
Here goes…
It’s been three months since Mark got hurt at work. It seems like we are just coming up for air. Though, he still has a long road of recovery ahead.
Mark wasn’t cleared by the surgeon to try to stand at therapy until 2 months after the surgery. He was completely NON-WEIGHT-BEARING and LEGS LOCKED IN EXTENSION for two full months.
Since blowing both tendons is so rare (even the health professionals kept forgetting the ramifications), there’s very little information on the internet about recovery.
Non-weight-bearing means a completely different thing when you have one good leg. Logistically and therapeutically.
Weeks 1 & 2: Care and Comfort
The first week was all about pain management, getting regular (KWIM), comfort and avoiding blood clots.
Since I was helping Mark with every single maneuver and task in the first few weeks, it was great that friends and family (who really couldn’t do much else for him) brought meals and gift cards for the local grocery store. It made feeding everyone easy on the fly. (It’s not even possible to express how humbled, grateful and relieved I was to receive this type of support so I won’t even try. If you know someone going through this, it’s an excellent way to help).
Mark was pretty much finished with the pain killers within 7-10 days.
The hardest thing for him was getting comfortable with both legs locked in extension in braces.
Mark also experienced an almost constant tingling, numbness and coldness in his feet, especially from the ball of his foot and toes. The kids or I would squeeze his feet with light pressure to relieve this as often as he asked. It gave him very temporary relief. Now that he’s on his feet more, he doesn’t notice it as much. At least it doesn’t bother him if it is there.
One dose of Senekot at night worked great to get the pipes moving that were jammed up from pain killers. ‘Nuf said.
Otherwise, good food, hot coffee in the morning, a captivating book and “The Sopranos” (loaned by a neighbor) kept things bearable in the beginning. We are so lucky to have the most thoughtful and generous friends and family. People were so supportive and thought of ways to ease the burden and this terrifying turn of events.
Blood Clots
Mark was on Lovanox shots (in the stomach-super fun) for 3 weeks post-op then 325 mg of aspirin 2X per day.
Ten days after he was finished with the Lovanox, he experienced a sudden onset of back pain (kidney/lower lung) in his left side. Accompanied by an occassional catching when he tried to take a deep breath.
No other classic symptoms associated with blood clots (swelling, other shortness of breath, chest pain). His symptoms improved with ibuprofen and lasted about 12 hours. We wrote it off as muscle pain or strain.
Two weeks later, the same pain returned in his back on the right side. This was more severe, lasted longer and again improved with ibuprofen. Since it was the second episode, we went to the ER. (No easy task when you can’t get into a car-grateful for a good friend who jumped in with his wheelchair van.)
Turns out that he had a clot in each femoral artery and pulmonary emboli in his right lung.
Long story not short, the hemotologist put him on 15 mg of Xarelto 2X per day for 3 weeks then 20 mg once a day until at least 3 months after he is completely mobile and unrestricted. He has had no problems on Xarelto.
My advice, don’t mess around with aspirin after the Lovanox. Insurance company will resist because it’s supposedly expensive but beg the surgeon to campaign for it or get a hemotologist to confer before you leave the hospital.
Hopefully you can afford the copay. If not, get to the ER as soon as you get whiff of a symptom, no matter how difficult it is.
Miscellaneous Comfort Tips
We realized a day or two after Mark got home that he got a lot of relief by laying flat and resting his legs on bed pillows long-ways. Sometimes two under each leg. It relieved pressure in his lower back and reduced swelling in his feet, ankles and legs. It also got his heels off the bed.
Mark iced his knees fairly regularly in the first two weeks. I left the hospital with the ice packs and covers plus refill ice packs. These 8 gel packs can also be heated and have come in handy for stretching once therapy started outside the house.
Therapy
Healing. That’s it. One week post op, Mark had an appointment with the surgeon to remove the surgical bandage. The next week he went back to get the staples removed.
Transportation
Mark was unable to get into or ride in a normal car or van. Even if he could have gotten in without levitating, he wasn’t allowed to bend his legs. We were lucky that the worker’s comp covered all transportation costs until he was able to get into a car. They sent a wheelchair van for all doctor visits and therapy.
Equipment
Here is a list of “MUST-HAVES“: Mark was injured at work and the Worker’s Comp carrier has been great about getting him everything he needs to help with his comfort and recovery. We are lucky NOT to have co-pays.
If you have high deductibles and are blessed with family and friends who really want to help, maybe they would be willing to help you afford these things for a few months.
- Urinal (get one before you leave hospital)
- Wash basin (again, hospital)
- Extra wide bedside commode (not the drop-arm model which would be a death trap)
- Ramp if you have stairs to the first floor of your home
- Sliding board
- Reclining Wheelchair (if possible)
- Case of wipes
- Fully automatic hospital bed (this is an affiliate link but you won’t likely be able to afford this. Insurance probably will. Campaign for the fully automatic. But get whatever you can.)
Since I cared for my aunt in our home for two years prior to Mark’s accident, we were equipped with a ramp into the house, a bedroom on the first floor with a fully automatic hospital bed and an extra wide bedside commode.
Let’s Talk About The Commode
Mark’s not a big guy so he likely wouldn’t have been approved for the extra wide commode (insurance approval is based on weight)-but we had one. Knowing what I know now, I would have paid the difference or bought one outright. It makes sponge-bathing himself so much easier and more comfortable. Since we don’t have a shower on the first floor or even a walk-in, this is important. Even if we had an accessible shower on the first floor, getting in there would have been virtually impossible with his restrictions in the first 8 weeks.
Also, Mark avoided a bed pan by learning how to maneuver onto the commode. Sorry for the graphic detail but this would be important to a person facing this injury.
How to Transfer When You Can’t Bend or Stand On Either Leg
Being locked in extension (legs straight out in braces) and non-weight-bearing, made transfers (even to a wheelchair or commode) tricky.
Luckily the hospital PT showed him how to slide onto the commode and wheelchair while his legs were still supported on the bed. He scooted sideways on the bed then backed into either chair. See photo below to see what I mean: (sorry for the blurry pic but gives you an idea).
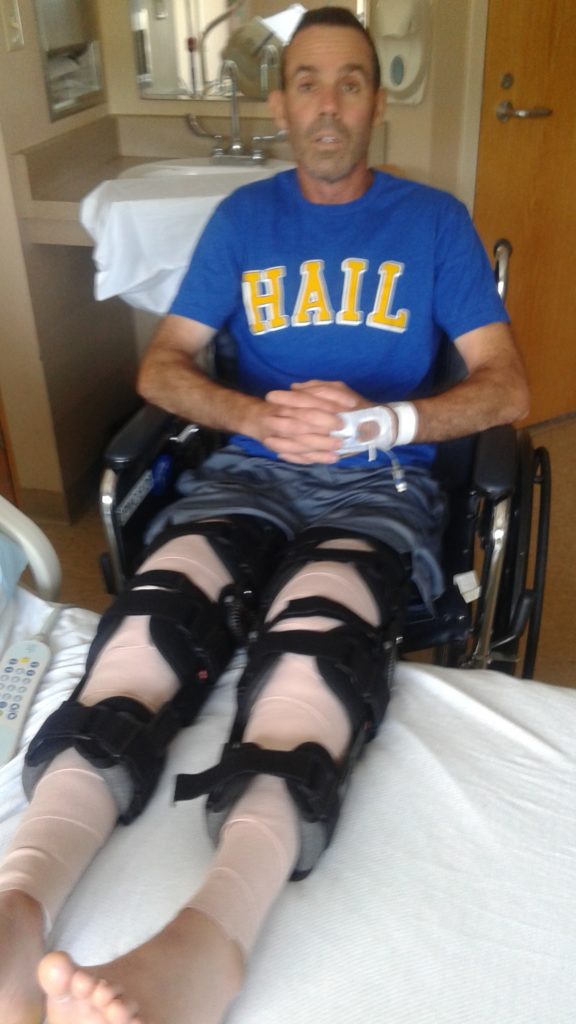
In the wheelchair, he would slowly back out while I supported his braced legs until the wheelchair leg supports could be swung into place (either by him or one of the kids-yes, a 3 man operation at first). Another trick was bridging the leg supports with 2 sliding boards so his legs wouldn’t fall through or have to be strapped to the supports. See photo below:
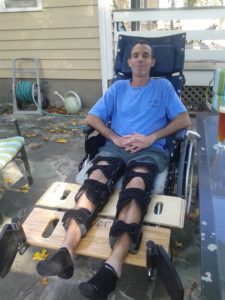
Reclining wheelchair and bridge for legs
We have a chair in the living room with a weirdly large ottoman. Both are low and were easy for Mark to slide onto from the wheelchair. (Photo below) If not for this furniture, Mark would have been stuck in bed or the wheelchair for 8 weeks.
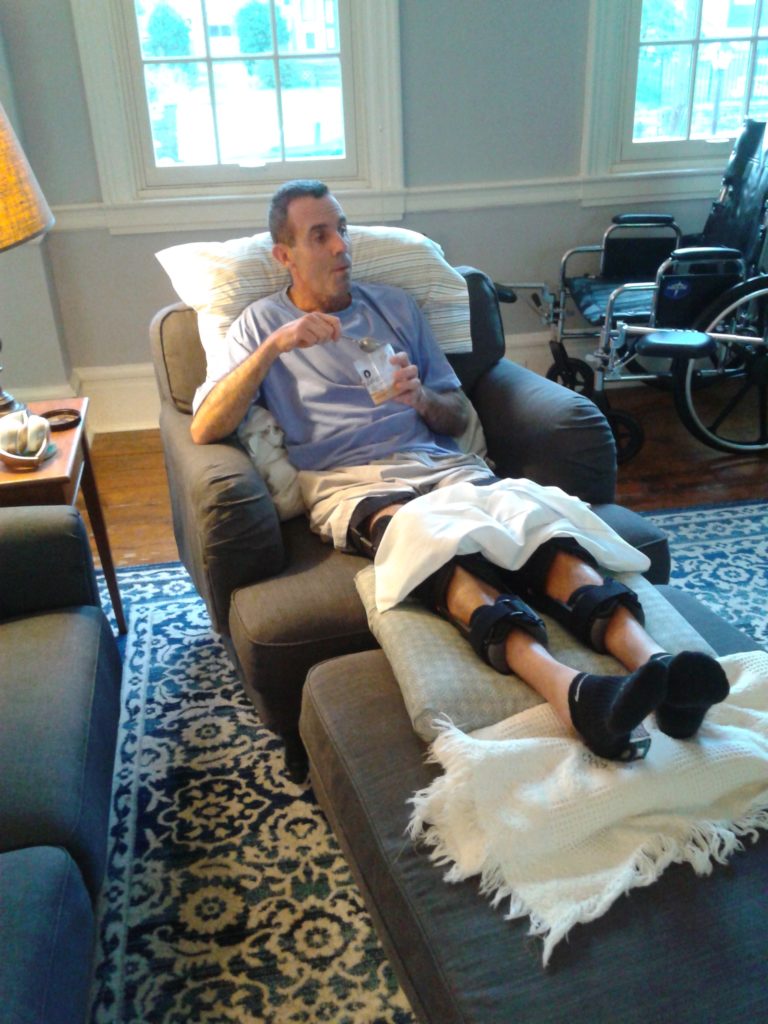
Let’s talk about the wheelchair for a minute.
The equipment company sent a lightweight wheelchair sized according to Mark’s height and weight. As much as I appreciated the size for maneuverability through the house, the narrow seat was uncomfortable for Mark since his legs were locked straight out in front of him. Imagine sitting upright in any chair with your legs straight out.
After a couple of tries, they found him a reclining chair which was much more comfortable for long periods of time (trips to surgeon, ER and in a wheelchair van).
The seat base is wide and deep and the ability to recline the back even a little makes a big difference. If you can get your hands on one of these bad-boys, even if you have to buy it yourself and resell it on Amazon when you’re finished, you won’t be sorry.
Hospital Bed
As I mentioned above, we already have a hospital bed because I cared for my aunt before Mark was injured. I’m guessing most insurance companies will authorize a hospital bed because they were asking if we would need one when Mark was still in the hospital. Get one if you can. If you can get a fully automatic one, get it. The bed made sleeping on his back bearable.
Mark didn’t need the trapeze so we sent it back. A bigger person might need one.
This post is getting loooong so I’ll tell you about the next 4 weeks post-op (weeks 2-6) in the next installment. I hope this has been helpful.
